|
May is Cystic Fibrosis awareness month. For a third year now, West Australian writer, Sandi Parsons, is helping to raise awareness through her 31 Days of Cystic Fibrosis. Despite CF: A Mother's Story For four and a half years, Merle Crawford took her daughter Carolyn back and forth to doctors. Despite a hospital admission for pneumonia and gastroenteritis when Carolyn was 16 months, doctors dismissed Merle's concerns. "One doctor thought I was fruit loop, and another told me I was having babies too quickly.” "The doctors at PMH didn't think there was anything wrong with her because she didn't look sick. They decided to put her on a fat-free diet, and when I went back, I told them it hadn't made any difference." Merle said. The next step was a sweat test, and Merle was told while they were not expecting a positive result, that someone would be in contact if there did prove to be something wrong. That call did come, and at the resulting clinic appointment with Dr. David Formby, Merle was told that Carolyn had CF. "Then David Formby turned to me and said to me, 'You realise she may only live a maximum of 16 years.' I nearly fell off my chair.” "They decided to take my two boys for the sweat test on them, but they were both clear. It was a relief, but the shock of Carolyn's diagnosis remained. I'd never heard of CF." The next step was learning how to do postural drainage in hospital. "Carolyn got upset wanting to know why I was hitting her. She asked why I was doing this when she hadn't been naughty. I explained to her that it was a problem with her chest. Explained that it was to help her, but in her mind, I was doing something awful to her." Carolyn's diagnosis affected the whole family unit. "It was a complete change of lifestyle; you had physiotherapy in the morning and at night. We got into a routine, the only thing I didn't like was mixing up the powder, the stinking rotten enzyme powder. It smelt like horse pee." Merle asked David Formby if enzymes were available in tablet form, but he brushed her off stating that Carolyn was too young. "Let me try," Merle said, "I gave her a demo and showed her how to take a tablet. I said hold your head back, and this big drink of water and they'll all run down your throat. And she mastered it. I went back and said I don't need this disgusting powder, can I have a script for the tablets?" With the removal of the enzyme powder, the household went from one foul smell to another. Carolyn needed to inhale mucomyst by nebuliser before every airway clearance treatment. "It was pretty rank," Merle said. "It stunk the whole house out." As Carolyn became a teen then an adult, the challenges became more confronting. "There were lung haemorrhages, and collapses. It was pretty frightening. I knew Carolyn was going downhill." When Carolyn was 26, Dr. Gerard Ryan, from the CF Clinic at Sir Charles Gairdner Hospital, suggested she should meet with the transplant teams from either Sydney or Melbourne. As the team from St Vincent's in Sydney, led by Dr Allan Granville was in Perth, it was an ideal starting point. Allan Granville told Carolyn "I estimate you have about two years left to live.” "It was like a bowling ball coming across the desk whacking you fair in the chest," Merel said. "And as it turned out, he was spot on." Instead of meeting with the Melbourne team for a second opinion, Carolyn put her faith in the team from Sydney. Both Merle and Carolyn moved to Sydney to start the long wait. Merle couldn't speak highly enough of the team from Sydney, the only hiccup being the need to navigate between two hospitals. The CF Clinic was held at RPA while St Vincent's was responsible for both pre and post lung transplant. After Carolyn had been on the waiting list for two years, Merle was given information that no parent wants to hear. Unless a transplant came through that weekend, the doctors would need to move Carolyn to ICU and intubate her. That would be the point of no return, for the team at St Vincent's would no longer consider Carolyn a viable candidate for transplantation. "I was freaking, but I didn't let her know." On Sunday Carolyn and Merle received the news they had been waiting for. The next period was frantic as they prepped Carolyn for surgery. Merle said, "Carolyn asked for the room, and she said, 'No matter what happens Mum you've been my rock. If I don't come back from this, don't be sad, because it will be a relief. But if I do - watch out!'” “Saying goodbye to let her go to the theatre was hard. Waiting to see her again was hard. But when I did, Carolyn held up her pink fingernails and pointed to her pink lips. She was as happy as Larry.” Allan Granville warned Merle that as Carolyn’s heart and other organs had worked so hard to keep her alive, one of the consequences would be a longer than normal recovery. “Yet sixteen days later, we were out. And I was in big trouble - Carolyn told me off for walking too slow. It was the first time she’d ever told me to hurry up.” In November this year, Carolyn will celebrate 27 years with her new lungs. By Sandi Parsons
0 Comments
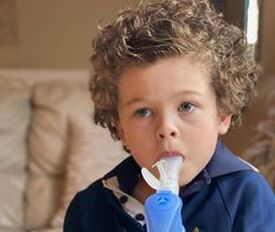
May is Cystic Fibrosis awareness month. For a third year now, West Australian writer, Sandi Parsons, is helping to raise awareness through her 31 Days of Cystic Fibrosis. Despite CF: A Son’s Story The implications of what CF meant for Harry Sippel’s mother became apparent at a very young age as he would accompany her to her various doctor and hospital clinic appointments. “My Mum is a very honest person and would tell me everything that went on with her health. That’s how you must be with such an erratic disease. Even though I was very young, I understood what my Mum had to do in day to day life.” Rather than struggling with this information, Harry found his Mum’s honesty empowering. “If something bad happened I wouldn’t know what to do or what was going on. If I didn’t know what was going on, why she did certain things, then I’d be angry.” “I played heaps of sport throughout my life, and thanks to my loving parents they always got me there. Sometimes I was a couple of minutes late for the game because I had to wait for my mum to finish her drugs. Most days, Mum would be there for me; however, if she couldn’t come, Dad would take me. That’s okay because I understood.” Having watched the ups and downs of CF, Harry’s experienced many emotions. “Over the years, I have been very scared and worried. However, my Mum is the toughest person I know. She taught me how to be positive when times are tough, which is easier for me to deal with it.” That positivity saw Kerry recently celebrate her 50th birthday. Harry said, dealing with his mother's CF’s is the reason he is tough and honest himself. “Everything in life is valuable, and every memory counts. Without my Mum, god knows where I would be today. She taught me how to deal with my type 1 diabetes. Life may throw many hurdles at you, but it’s how you jump those hurdles that really counts.” By Sandi Parsons
May is Cystic Fibrosis awareness month. For a third year now, West Australian writer, Sandi Parsons, is helping to raise awareness through her 31 Days of Cystic Fibrosis. Despite CF: A Mother's Story For the first 24 hours after Connor's diagnosis with CF, Taryn Barret felt a mix of shock and disbelief. All Taryn knew about CF was, "Horror stories, I didn't think Connor was going to have a good quality of life - I'd look at him and picture the worst." Meeting with the CF team at Princess Margaret Hospital was a turning point, and she came to have a better understanding of the disease and its implications. It was after this meeting that Taryn could look at her son and think, "Yes, Connor is going to have a great life." To date, Connor hasn't needed hospitalisation for IV antibiotics. Early on, Taryn established a routine to ensure that treatments were given priority with physio completed twice a day. This non-negotiable routine has helped with Connor's compliance regarding physio. "I hope this has attributed to him being really well, and while I know that could change at any point, it's something that works for our family," Taryn said. Some people with CF decline earlier than others, and while Taryn is optimistic, the death of a young person from CF always hits hard. In counterbalance, Taryn finds perspective from talking to adults with CF, "They just get on with things and have a positive perspective on life." Taryn feels fortunate that Connor has access to the breakthroughs that have been funded by the generations of research done in the past. "I feel like we are really lucky given that now there has been a turning point, and there is so much hope for the young kids - particularity with the new Vertex Pharmaceutical medications - we're not there yet, but there is hope." Taryn is a committee member for Conquer Cystic Fibrosis ; an organisation run entirely by volunteers. Taryn sees the need for research to be the primary focus in the fight against CF. She hopes there could be advancements that will enable Connor to have a long life, and even grow old. Conquer Cystic Fibrosis channels the majority of its fundraising monies into research therefore, it was a natural fit for Taryn. Through her charity work, along with her former work in both journalism as well as working for a Member of Parliament, Taryn is well aware of the power of advocacy. Orkambi was a medical breakthrough and among the first medications to treat the underlying causes of CF instead of the symptoms. However, inclusion on the PBS wasn't automatic. Taryn's passion for advocacy during the campaign to see Orkambi listed on the PBS saw her awarded the Patron Award for CF Consumer Advocate in 2017 by Cystic Fibrosis Australia. Now Taryn is setting her sights on Trikafta — a new, improved modulator that has the potential to see Connor live a normal life. Taryn, spoke at the Capel Vale Conquer Cystic Fibrosis Grand Ball 2017 – you can hear her speech here: https://www.youtube.com/watch?v=4gdDiWXXhV8 By Sandi Parsons
May is Cystic Fibrosis awareness month. For a third year now, West Australian writer, Sandi Parsons, is helping to raise awareness through her 31 Days of Cystic Fibrosis. Despite CF: A Wife’s Story For Natalie Cahill the topic of CF came up on her first date with Michael. “It was the first time we had gone out - we were eating and Michael took his creon. I asked him what they were for and he said, ‘I have Cystic Fibrosis’. I googled it when I got home and it came up with the worst information. As our relationship developed I learnt more about CF from Michael.” CF affects people in different ways, and Natalie initially thought a relationship with a person with CF would be harder. “Apart from when he is hospitalised, the rest is simply the way things are in our house. Very few times has it stopped us doing anything a non-CF house does.” The decision to start a family, however, was one of those times. Although men with CF can father biological children, for most men with CF, fertility assistance is required. “We had to conceive through IVF. Our miracle daughter Zoe was conceived on our 11th cycle.” Natalie is very pragmatic about the challenges of life with CF. “When Michael is hospitalised, I have to balance seeing him and getting Zoe to school for her after school activities to keep her life ‘normal’. We do have family that can help out where possible. Nothing in life is guaranteed, so I go with it and what life throws at us as a family. We are lucky Michael is pretty ‘healthy’. Which has allowed us to travel a little.” “Michael is an incredible person - he isn't CF, but it is a part of him. He has a strength that amazes me every day. Along with the ability to get on with life no matter what CF throws at him. Michael always looks after Zoe and I while balancing work and going to the gym to keep healthy and fit.” By Sandi Parsons
May is Cystic Fibrosis awareness month. For a third year now, West Australian writer, Sandi Parsons, is helping to raise awareness through her 31 Days of Cystic Fibrosis. Despite CF: A husband’s story John and Kate Rootsey have a normal family life with their six-year-old daughter, Molly. Like any family, they are busy day-to-day taking Molly to her various activities and often go away on holidays – but having a family wasn't originally part of their plans. When John met Kate after her double lung transplant, he was unaware of CF and its implications. He asked all the common questions. Kate told him that despite her transplant CF complications remained – in particular in the digestive system , and that due to her transplant the possibility of children was unlikely. Furthermore a life with her would present challenges, but John knew they could face them together. However, with the blessing of the Lung Transplant team at Prince Charles Hospital, John and Kate embarked on a three-year journey to have Molly. It was new territory for everyone involved; as Kate was the first woman in Queensland to have a baby after a double-lung transplant. As a high-risk patient, Kate was first required to change her anti-rejection medication. Immunosuppression levels need to be fine-tuned to continue to reduce rejection in the lungs and also be a safe level for fetal development. Their three-year journey contained numerous appointments, blood tests, and two miscarriages. John describes this period as a “Very scary and exciting time, as we weren't sure how the possible outcomes could affect her.” Having to deal with so many difficult situations has made Kate an extremely tough person, and John says it makes him not only appreciate both his own and his daughter's health but also to make the best of any situation. BONUS FACT: John’s top tip – Do NOT eat like a CFer.
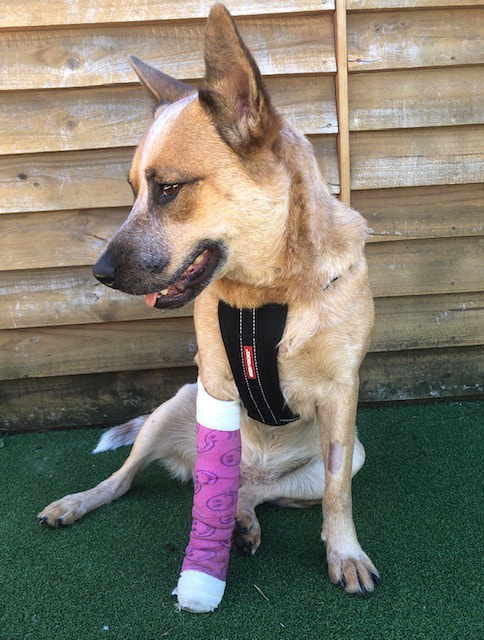
May is Cystic Fibrosis awareness month. For a third year now, West Australian writer, Sandi Parsons, is helping to raise awareness through her 31 Days of Cystic Fibrosis. Sandi's piece below is published on Medium. 5 Lessons Medical Practitioners Can Learn From Veterinarians My red heeler, Chilli, recently came off second best in a rumble with my staffy cross, Rotto. An ordinary trip to the vet triggers deep anxiety within Chilli. She is, even on her best days, a nightmare of a patient. She’s the type of dog that makes trainee veterinarians second-guess their career choice. An emergency vet trip, combined with pain and significant blood loss, saw Chilli morph into a whirlpool of emotions and gnashing teeth. With thirty kilos of agitated dog twirling around spraying blood, it looked like Stephen King had taken over and blended Carrie with Cujo. Nonplussed, the staff did everything possible to make Chilli feel safe so they could stop the bleeding. It’s the same at my regular vet clinic. Everything is designed around making the patient feel comfortable and at ease. Why don’t medical practitioners work to the same method? And what can they learn from veterinarians? 1. The patient should always be number oneLiving with Cystic Fibrosis and a compromised immune system due to a lung transplant, I am at an extremely high risk of contracting an airborne respiratory virus. (I’m not just pointing the finger at you, COVID-19). In 2012, my lung function was compromised. It was my first major infection since I’d traded in my manky old lungs. My donated lungs needed a little medical intervention to help them do their job. An orderly collected me from the respiratory ward, and, on arrival at x-ray, he parked my wheelchair next to a yellow carded patient. In the Western Australian hospital system, a yellow carded patient means they have an airborne respiratory illness. You don’t need a medical degree to join the dots and figure out this was a less than ideal place for me to sit. My polite request to be moved was just as politely ignored. I learned to navigate the hospital system at an early age. There was only one advocate that had my back. Me. My performance was worthy of an Oscar. As there was nowhere else to ‘park,’ I ended up sitting tucked in an alcove out of sight. I’m pretty sure the staff made me wait longer because I’d morphed into a germophobic nightmare for them. Still, it was a safer option than sitting next to a yellow carded patient. (Thank you, COVID-19, for educating people on the hows and whys of airborne contagions, so I no longer have to seem like a germaphobe.)
In contrast to the Australian public health system, my vet clinic has four consulting rooms with only two vets on shift. That leaves two rooms for nervous or aggressive dogs to wait separately. Chilli’s patient file has a permanent note attached about her anxiety. It may even have a note about her germophobic owner — but that doesn’t matter because Chilli is treated better than the Queen’s corgis on arrival at the clinic. We’ve been frequent flyers lately due to multiple pressure bandage changes. And we’ve gotten into a bit of a routine. Chilli and I sit in our own private room. The vet enters quietly, speaks in a soothing voice, squats down at Chilli’s level, and pets her. After the administration of Chilli’s sedation, the lights are turned off, and we’d be once again left alone. When Chilli succumbed and finally nodded off into her twilight sleep, the vet would return. The door was always left open, and the vet would change her bandages in the dim light as both light and loud noises can ‘wake’ a sedated dog. As the patient, Chilli is always the number one priority in the room. 2. Health is a service industry, but no one has informed medical staff My transplant team includes three consultants. Leaders in the field of respiratory medicine. However, because my hospital is a teaching hospital, doctors regularly rotate through the Advance Lung Disease Clinic. Minions. They’re there as part of their training to learn about various medical disciplines. Often the minions are ticking a box to finish their studies or as an entry requirement into another discipline. A consult with a minion is like ticking boxes, too — you never want to bring up the big stuff because they can’t make decisions. Instead, they need to go and consult their Leader. In the raffle lottery of patients' files, a minion plucked mine from the stack of medical tomes. As he gazed across the clinic, the number of people sitting like herded cattle in the waiting room caused the minion some concern. He glanced at his watch and frowned. Consequently, he rushed through my consultation. At the end, when I presented him with a list of medications I needed new scripts for, he brushed me off. “I don’t possibly have time to call for an authorization number for these scripts. Haven’t you seen the waiting room? I’ll do it this afternoon and post it to you.” Without leaving me time to answer, he strode out and called his next victim in. Back in the waiting room, I promptly rang the minion’s Leader and turned on my Oscar-worthy charm. The cocktail of pills I pop is finely tuned and causes chain reactions, as they link hands and dance throughout my body. When one link crumbles, the risk is akin to a tumble in the middle of the Dirty Dancing lift. With one weak link, it was critical to refill that medication urgently. A situation that a simple question could have avoided. “Are there any medications on this list you need urgently?” Goodwill is the single reason I’ve used my vet practice for the last 29 years. I’ve moved house many times, and there are several closer options. All have a solid reputation. Yet, I return to the same practice because the service is always outstanding. But the possibility always remains that if I become unhappy, I might choose to jump ship.
Goodwill is a huge part of any business, and all the staff at the vet practice factor this into all their client transactions. Their service is not only outstanding at the time of the visit but also in the follow-up. Whenever one of my dogs has been for a procedure, the following day always brings a text or phone call asking after my dogs’ welfare. Vets stop to talk to their patients, soothe them, and take the time to pet them before they start examinations. It’s all too easy for a frightened animal to turn aggressive. Animals are unpredictable and can snap quickly. Vets treat the patient, not the waiting room. 3. Treatment methods are presented as options“If you don’t start taking your blood pressure seriously, you’re going to die.” It was said in the I am a doctor and I know what I am talking about voice. The one doctors with a god complex always use. It’s usually annoying. But from a minion, it’s insulting. Ultimately, it was a tactic designed to scare me into compliance. I was supposed to act like a good girl and take the medication without asking questions. However, the minion with his god complex failed to consider that I’d been to all the previous meetings about my blood pressure issues. I was well versed in my own history. I’d been through the dress rehearsal already. This blood pressure medication had already failed to dance nicely with others. It turned my finely tuned waltz into the jitterbug. The issue wasn’t as simple as popping that particular pill. I didn’t need a lecture. I needed a workable option. The minion went to consult his Leader and came back with a new, improved plan. Eventually, after a few mishaps with the cha-cha-cha, I played with the timing of my medications. There was a period of moonwalking before I finally solved the interaction issues and got my waltz back on track. There was, however, no point when I wasn't taking it ‘seriously.’
There is no good way to deliver bad news. In 2018 my blue heeler, Pepsi, was diagnosed with canine cancer. My husband and I were given multiple options—the pros and cons of each option carefully presented to help us make the best decision.
Ultimately the decision was ours. My husband and I chose palliative care and gave Pepsi a bucket list (okay, that was mainly me — but who’s to say dogs don't dream about bucket lists … ice-cream in the park, the whole pizza, not just the crust …). At no point did anyone at the vet practice attempt to talk us into another option. It was never about money. The issue was always about what would be best for Pepsi. We knew what was best for our dog, and our vets respected our decision. 4. End of life optionsThe euthanasia debate will always be controversial. But until you are in that position, you have no idea what you will want or if your fixed mindset views will change. Here’s what I do know. I was mere weeks away from dying when an offer of donated lungs saved my life. Dying from respiratory failure is a slow, brutal way to die. It is not a waltz that leads you off into the sunset with slowly fading music. It is the most degrading thing I’ve ever endured. There is no dignity when you are slowly dying. I lived through that experience because I had hope. I had faith in my fellow humans that an offer of donated lungs would come. I did everything I could to stay alive long enough to get that phone call. In the end, I was hanging on by my fingernails. Sheer willpower alone kept me breathing. Next time around, when these wonderful lungs eventually fail me, there will be no lifeline. There will be no hope. There will be no phone call. At the end of the pain, the indignity, the loss of everything I hold dear, I will die. I may want an out. At a time and place of my choosing. To let the waltz fade into the sunset after all. Legislation in Australia is slowly evolving. And I may get that out. But it needs to be my choice to make.
One Friday, our bouncing girl ran through the house demanding her breakfast. But in the afternoon, Pepsi’s tumor grew the tiniest bit larger, and it pushed a little harder against her brain. Without warning, we became unable to control Pepsi’s pain. With a single look, my husband and I knew that the next day would be her last. We gave her the highest dose of pain relief available to help her sleep. Keeping Pepsi alive at that point would have been for our benefit — not hers. On Saturday morning, Pepsi had pancakes for breakfast. My husband cooked a Jamie Oliver recipe for lunch, and outside the vets, she had her final bucket list treat. White chocolate — a treat she’s always wanted to try. No one at the vets second-guessed our decision. No one tried to talk us out of ending Pepsi’s life. Instead, they treated her with dignity as she took her last breath. 5. Yes, please to the tasty treatsI’ve seen TV shows where pediatricians give patients a lollipop at the end of the consult. The Friends episode where Ross bounds out after his appointment with his pediatrician is one that immediately springs to mind. But I’ve never once had a doctor offer me a lollipop. Instead, I’ve been given scripts for fistfuls of medications, sample pots for me to provide specimens, x-ray forms, or instructions for procedures they wish me to undertake. Just once, it would be nice to get a tasty treat like my dogs do when they visit the vet. A tasty treat often makes everything better. Of course, there is one habit I don’t want my medical practitioners to pick up from veterinarians. At all costs, keep that thermometer away from my butt! By Sandi Parsons
May is Cystic Fibrosis awareness month. For a third year now, West Australian writer, Sandi Parsons, is helping to raise awareness through her 31 Days of Cystic Fibrosis. Despite CF: Brooke Austin After a tough and exhausting pregnancy, three pulmonary embolisms sparked an emergency drama for Brooke. She underwent an emergency caesarean five weeks before Henry's official due date. Brooke's mother died after a pulmonary embolism. In a series of overwhelming coincidences, Brooke was facing a similar situation. "That was very frightening. I think I recovered pretty well. My specialist ended up keeping me in for a tune-up for almost 2 1/2 weeks because he said I'd need a boost after everything." Nonetheless, despite the dram, Brooke managed to make it to 40 while still quite healthy. Looking to the future, Brooke has a fixed plan. "Up next? Continuing being the best Mum & Wife and enjoying my life! CF will not stop me! By Sandi Parsons
May is Cystic Fibrosis awareness month. For a third year now, West Australian writer, Sandi Parsons, is helping to raise awareness through her 31 Days of Cystic Fibrosis. Despite CF: Kate Hooke After completing an Honours degree in social work, Kate gained a position with a not-for-profit in NSW. At the peak of Kate's social work career, she worried that CF might exclude her from promotion. The need to work a four-day week was crucial for maintaining her health. Regardless of her worries, Kate was the best person for the job. "I loved this role, and I am immensely proud of what I achieved while working in it." Not one to let CF stop her, Kate has sailed a yacht from Sydney to New Zealand and walked 50kms from Balmoral to Coogee in Sydney. Both are feats that require a level of determination to accomplish. Kate later set that determination to a different focus when she took on the NDIS. Even when her application was denied repeatedly, she persevered. "With valuable help, I went to the AAT and challenged the NDIA on their decision. They sadly settled with me rather than the AAT making a judgment — which would have enabled other people with CF to gain access." Kate has since used her experience to successfully provide others with CF information about the route to access NDIS funding. Having just turned 50, Kate has found herself in a holding pattern. "My lung function is in the mid 40's so I'm working hard to maintain what lung function I have." "I was gutted when Trikafta was deferred as I'm looking forward to trying it, and if I'm lucky enough that it does work for me, I can start the next chapter of my life." That next chapter goes hand in hand with Kate's desire to see her teenage son grow up. "He is an amazing teenager - as amazing as 14-year-old boys can be anyway! I love him to pieces, and he is a great motivator for me to stay as well as I can." Kate's crossing her fingers that she can watch her son finish his education, return to her career, and maybe become a Grandma one day. All she needs is a little help from Trikaffta. By Sandi Parsons
May is Cystic Fibrosis awareness month. For a third year now, West Australian writer, Sandi Parsons, is helping to raise awareness through her 31 Days of Cystic Fibrosis. Despite CF: Adrian Flor Adrian Flor has a motto for balancing life, work, and CF. "Never feel like you can't at least give something a go." Adrian's life is always busy: — there's his health to maintain (CF along with the complexities of CFRD), a 12-year career as a lawyer, daily exercise, and family responsibilities. Family is, of course, the most important — "I'm part of a beautiful family. I'm married to the most supportive wife who has made me an immensely better person. It sounds cliche, but I wouldn't be who I am without her. I also have the sweetest and liveliest son (conceived through IVF)." Exercising keeps Adrian healthy, and he uses a mix of weights and running in his fitness regime. As an exercise nut, Adrian's current goal is to beat his last FEV1. "My last FEV1 was 105%, and I'm aiming to better that - I always try to improve!" By Sandi Parsons
May is Cystic Fibrosis awareness month. For a third year now, West Australian writer, Sandi Parsons, is helping to raise awareness through her 31 Days of Cystic Fibrosis. Despite CF: Gemma Chloe Gemma needed a liver transplant when she was in Year 8. "It took a long time to recover. There was a stage where I was questioning if I should drop out in Year 10." Despite these doubts, Gemma continued with her education, eventually completing Year 12 and graduating High School. Living with CF continued to be a struggle, and in 2013 Gemma had a double-lung transplant. Finally, Gemma was well enough to continue her education. "I was always too sick to complete university or any other courses. I finished my Certificate IV in Floristry after my double lung transplant." Gemma also competed in the City to Surf after her double-lung transplant. "Doing the City to Surf with new lungs was one of the best feelings. It was great being able to achieve that without struggling to breathe." Post-COVID Gemma and her long-term partner are hoping to travel overseas — "I would love to go to Ireland, Scotland, and the UK." By Sandi Parsons
|
Disclaimer
The Australian CF Hub strives to present a diversity of viewpoints. We encourage respectful and open discussion. The views, thoughts, and opinions expressed in each blog post belong solely to the author, and do not necessarily reflect the views of the Australian CF Hub team or other adults with CF. Archives
May 2021
Categories |










 RSS Feed
RSS Feed
